
Pregnancy is an exciting time that's full of anticipation, but it also involves some significant changes to your body. One change you may not be expecting, however, is little bladder leaks. You may have noticed that everyday activities like laughing, coughing, sneezing or exercising now result in some dampness in your underwear. Incontinence during pregnancy is common and something many expectant mothers experience. The fact that something is common doesn’t mean that it is normal, please don’t simply put up with it!.
Table of content:
- What are the causes of incontinence in pregnancy?
- Types of incontinence in pregnancy
- What are the risk factors for incontinence in pregnancy?
- When in pregnancy are bladder leaks most likely to happen?
- Incontinence in pregnancy: a typical timeline
- How to manage and prevent leaking urine during pregnancy?
What are the causes of incontinence in pregnancy?
Pregnancy is a unique period during which a woman’s body undergoes numerous anatomical and hormonal changes, preparing for childbirth. These same changes can also increase the change of bladder leaks during pregnancy.
The most common causes of incontinence include:
- increased urine production due to higher blood volume, which causes the kidneys to filter more of it, so the bladder therefore has to empty more often;
- pressure from the growing uterus on the bladder - as pregnancy progresses, the growing uterus moves upwards and forwards, putting pressure on the bladder, which limits its capacity and promotes leakage, especially in the third trimester;
- hormonal influence - progesterone and relaxin loosen muscles, ligaments and joints, preparing the body for childbirth. At the same time, they weaken the pelvic floor muscles, which have a role in controlling urination;
- constipation increases abdominal pressure – frequent bowel problems during pregnancy further strain the pelvic floor muscles, increasing the risk of stress urinary incontinence;
Types of incontinence in pregnancy
The most common form of pregnancy incontinence is stress incontinence – involuntary bladder leaks that result from a weakened pelvic floor. Your pelvic floor is the system of muscles, ligaments and tissue that supports your bladder, uterus and anus. If the pelvic floor muscles are unable to fully support the bladder, urine leaks can occur during activities that increase abdominal pressure such as coughing, laughing or exercise.
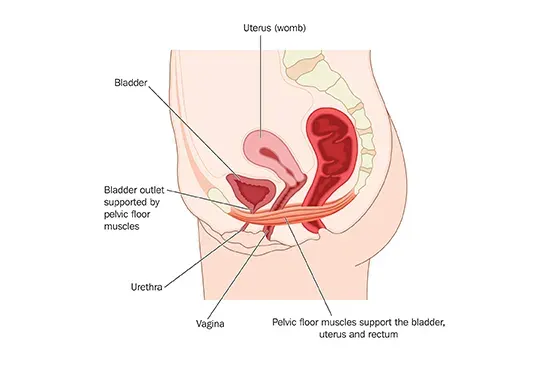
The key to minimising stress incontinence urinary leakage during pregnancy is to practice pelvic floor exercises. In some cases, incontinence during pregnancy is caused by an overactive bladder, also known as urge incontinence. Here there is a sudden and intense need to pass urine and you might not get to the toilet in time. During pregnancy this is often related to bladder sensitivity and pressure from the uterus, which may cause bladder spasms or frequent urges.
What are the risk factors for incontinence in pregnancy?
Urinary incontinence is common during pregnancy, but not all women experience it. Certain factors can increase the likelihood or severity of symptoms.
- Older maternal age - pelvic floor muscles and tissues gradually lose elasticity and strength, making it difficult to maintain proper muscle tone around the bladder;
- Having obesity or overweight - additional weight increases intra-abdominal pressure, which strains the bladder and the muscles supporting its function;
- Previous vaginal delivery , especially with severe tears that weakened the pelvic floor or damaged the nerves around the bladder - may lead to stretching, weakening, or damage to the pelvic floor muscles, as well as the nerves controlling urination;
- Smoking, which leads to chronic coughing - persistent coughing increases pressure on the pelvic floor, and nicotine also impairs tissue blood flow and regeneration;
- Gestational diabetes, which can affect your nerve function - may affect nerve function, leading to impaired sensation and bladder control.
- History of Incontinence - Leaking urine before or in past pregnancies is a strong predictor that it might recur during this pregnancy
- Constipation: Straining from chronic constipation puts pressure on pelvic
- High Birth Weight Babies - Larger babies increase pressure on the pelvic floor during delivery.
- Physical Activity - Intense weightlifting or heavy lifting can strain pelvic floor muscles.
- Urinary Tract Infections (UTIs) - Can worsen incontinence symptoms.
If you do develop urine leaks in pregnancy please discuss with your antenatal team, and if it is accompanied by pain, burning on passing urine or fever please seek medical advice.
When in pregnancy are bladder leaks most likely to happen?
Pregnancy doesn’t just affect your uterus, but the whole body including your urinary system. While urinary leaks are common, remember they are not simply normal and should be addressed.
- First trimester: In the early weeks, many women experience frequent urination due to hormonal changes that increase blood flow through the kidneys and boost urine production. At this stage, your uterus is still low in the pelvis and competes for space with the bladder, meaning you may feel you go more often.
- Second trimester: After around the 12th week, the uterus rises into the abdomen, relieving some pressure on the bladder. As pregnancy hormones like progesterone and relaxin loosen muscles and ligaments, the pelvic floor may begin to weaken.
- Third trimester: As your baby grows and moves into position for birth, their head presses directly on your bladder, significantly reducing its capacity. Many women find that any sudden movement, sneeze, or even change in posture can cause small leaks. The added weight of the baby and higher intra-abdominal pressure make bladder control even more challenging.
Don’t worry, many people notice that symptoms improve after delivery as the pressure is relieved off the bladder and the pelvic floor can strengthen again. But, don’t ignore it, ask for help and regularly practice your pelvic floor exercises to control your symptoms and reduce the risk of leaks in the future.
How to manage and prevent leaking urine during pregnancy?
Just because pregnancy incontinence is common, doesn’t mean that you need to be uncomfortable. There are a number of tips and tricks that can help prevent or reduce the severity of your symptoms and assist postpartum recovery.
-
Pelvic floor exercises - You may know them as Kegels. Performing Kegel exercises strengthen the pelvic floor muscles so they are stronger and more successful at holding in urine, preventing bladder leakage during pregnancy. Read how to perfect your pelvic floor routine here. Depending on where you live you may be able to self refer to a women’s health physiotherapist or your GP may be able to refer you for support.
-
Toilet habits - If you need to go, go, don’t routinely delay going but also don’t force urination or go just in case, only when you need to. Also avoid stopping passing your urine mid way, when you go, go!
-
Diet - A high-fibre diet supports proper bowel function and prevents constipation, which is common during pregnancy , straining increases pressure on the pelvic floor. Your local pharmacist, GP or midwife may be able to advise you on laxatives if needed. It is also important to limit artificially sweetened caffeinated beverages (soft drinks, energy drinks, sweetened juices), as sweeteners and caffeine irritate the bladder, increase urination, and may worsen dehydration, paradoxically intensifying incontinence.
-
Don’t forget protection! - Wear a sensitive liner or pad to protect your underwear and to keep you feeling fresh, clean and comfortable. Incontinence products are specially formulated for urine loss, whereas the traditional feminine hygiene products you might use for your period are formulated for menstrual blood, which is more viscous than urine. Incontinence liners and pads absorb leaks and odours within seconds, keeping you dry and protected, so that you can successfully manage your pregnancy incontinence for an enjoyable and comfortable pregnancy. Incontinence pads and liners are not treatments for bladder leaks, but can help keep you comfortable while you seek advice and treatment.
